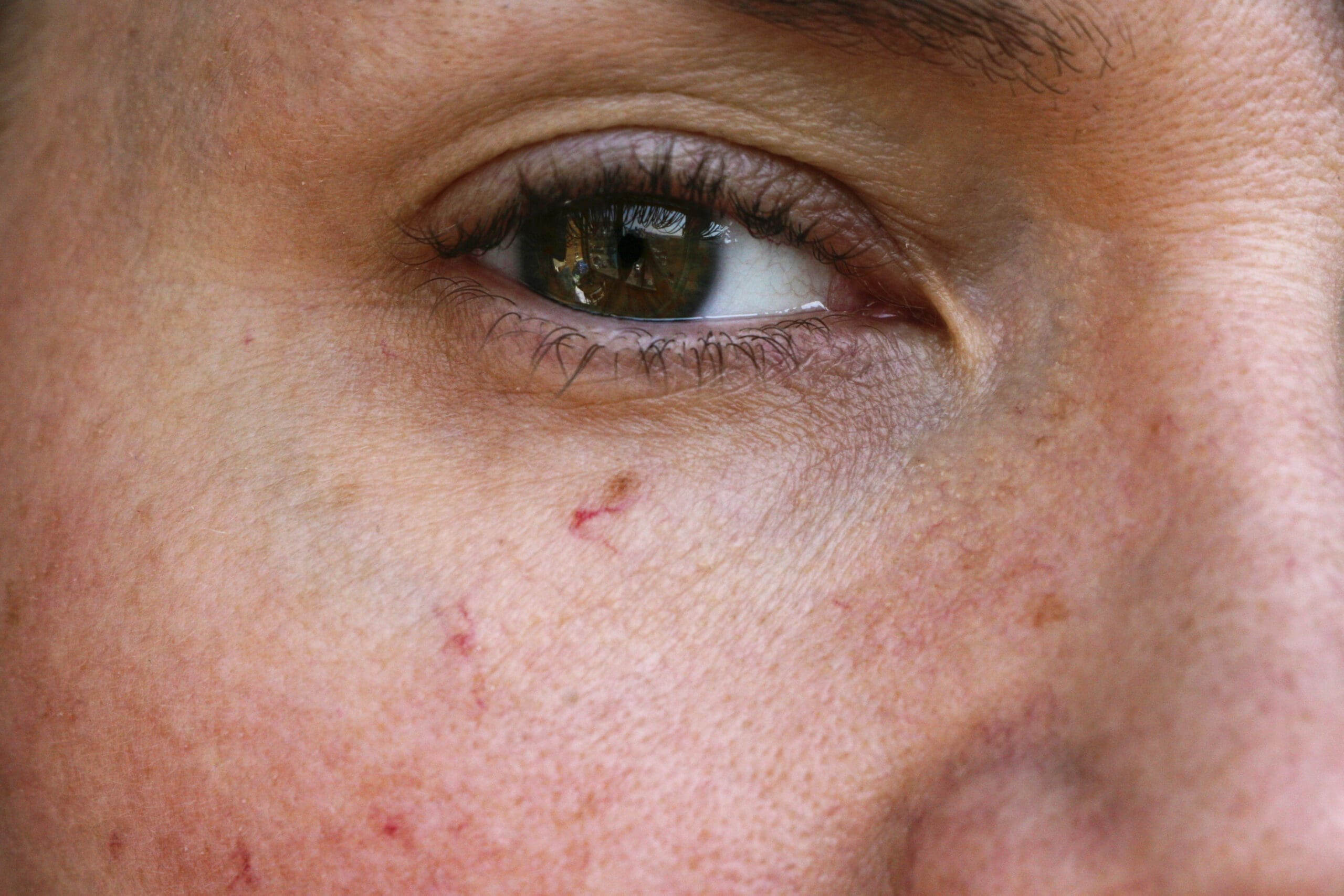
What is hereditary haemorrhagic telangiectasia?
Hereditary haemorrhagic telangiectasia (HHT) is also known as Osler–Weber–Rendu disease or Osler–Weber–Rendu syndrome.
Hereditary haemorrhagic telangiectasia is a rare inherited condition affecting blood vessels throughout the body. The vessels do not develop properly and it causes haemorrhage (bleeding) between arteries and veins. This is called arteriovenous malformations (AVMs). AVM’s can be life threatening if haemorrhage occurs in the brain, lungs or gastrointestinal tract (stomach and intestines). 1 2
Approximately 1 in 5,000 -10,000 people worldwide inherit the disease. 3
What are the symptoms of HHT
Symptoms of hereditary haemorrhagic telangiectasia vary, depending on the specific gene. They can happen at any age group. 4
Usually the first symptom is epistaxis (nose bleeding) during puberty, this is caused by small, red lesions (telangiectasia) of the mucous membranes in the nose. Legions can appear on the fingers, face, lips, tongue and ears. 5 6
The organs affected by hereditary haemorrhagic telangiectasia and the symptoms can be seen in this table.
Hereditary haemorrhagic telangiectasia symptoms
| BODY ORGAN | SYMPTOMS |
| Gastric | Pale skin, Abdominal pain, Abdominal swelling |
| Lungs | Shortness of breath, Difficulty breathing, Coughing blood |
| Liver | Whiteness around eyes, Yellowish Skin |
| Spinal Cord | sleepiness, Vomiting, Back arching, Seizures, Urinary retention |
| Heart | Chest pain, Bluish discolouration of skin (cyanosis) |
| Brain | Fatigue, Headaches or Migraines, Loss of Consciousness |
Causes
Hereditary haemorrhagic telangiectasia is a genetic disorder. It is inherited from a parent. There is only one gene needed for it to cause hereditary haemorrhagic telangiectasia and this is called a dominant gene.
At least five different genes can cause hereditary haemorrhagic telangiectasia, four of which are known. These four are endoglin, activin A receptor like-kinase type, bone morphogenetic protein receptor type 9, and mothers against decapentaplegic homolog 4. 1
In the offspring of a person who has hereditary haemorrhagic telangiectasia, there is a 50 per cent chance of inheriting the gene. 9
Risk factors
Hereditary haemorrhagic telangiectasia increases the risk of both bleeding and embolism (clotting). This can occur in any place of the body where there is telangiectases and an AVM. 6
- Bleeding risks from hereditary haemorrhagic telangiectasia in the body can present in the form of blood in sputum, nasal mucosal, cysts or polyps, they can also appear as abscess, haemothorax (blood in between the chest wall and lungs), spinal haemorrhage and cardiac shunt (right-to-left side blood flow through broken heart wall). 6 10
- AVM risks from hereditary haemorrhagic telangiectasia can affect several organs of the body and problems with their function. These include the stomach and small intestine (gastrointestinal), the liver (heptic), the lungs (pulmonary) and the spine. It can also present itself in the heart (cardiac issues) and brain (cerebral issues) 1 6.
Clotting risks from hereditary haemorrhagic telangiectasia in the body are:
Tests and diagnosis
Hereditary haemorrhagic telangiectasia is diagnosed by using ‘The Curacao Diagnostic Criteria’.
The Curacao Diagnostic Criteria for hereditary haemorrhagic telangiectasia
| DIAGNOSIS | |||
| CLASSIFACTION | Unlikely | Possible | Definite |
| Criteria | Less than two | Two | Three |
The Curacao Diagnostic Criteria:
1. Spontaneous and recurrent nosebleeds.
2. Telangiectasias at multiple and specific sites.
3. AVM or telangiectasia of internal organs (lungs, brain, spinal cord, liver, stomach and intestines)
4. Family history of hereditary haemorrhagic telangiectasia (parent with dominant gene). 12
Hereditary haemorrhagic telangiectasia can be investigated with CTI (Computerised tomography scan) and MRI (Magnetic resonance imaging) scans, Endoscopy/colonoscopy of the bowel and a pulmonary shunt study (ultrasound with bubble study) 4.
Management and Treatment
Gentle oral hygiene will help prevent lesions occurring.
Nosebleeds can be stopped by applying pressure to the part of the nose (above the nostrils) for 10-15 minutes and breathing through one’s mouth while leaning forward. Intranasal avastatin topical spray can reduce nosebleeds. 1
A diet sufficient in iron is important to prevent anemia.
If a blood test shows an iron deficiency, it can be corrected with blood transfusion, iron supplements and folic acid. 4
Prescribed antiangiogenic (reduce blood vessel growth) and antifibrinolytics (stop clotting) are given to reduce bleeding. Antiplatelet therapy is only used when someone has cerebral or coronary artery disease. 4
Estrogen and/or progesterone therapy prevents recurrent bleeding. 4
Migraines are managed with paracetamol and in some severe cases, infusion therapy.
Low dose aspirin and heparin can prevent clots. 11
Antihypertensive medications reduce problems with high blood pressure.
Surgery
Surgical interventions are sometimes needed to correct AVMs. These can be in the form of a non-contact laser therapy and nasal packing or a septodermoplasty, sometimes you may require a gastrointestinal tract endoscopic or laparoscopic / laparotomy.
Based on your condition doctors may also choose a liver transplant, cardiac surgery, surgical resection of lung or brain or a percutaneous catheter embolisation or a gamma knife. 1 9
Before your procedure your specialist will discuss these options, and the one that is right for you, in detail.
Team of specialists
The best management of hereditary haemorrhagic telangiectasia is with a team of experts. Consultation between the General Practitioner, Ear Nose and Throat (ENT) Specialist, Pulmonary Specialist, Radiologist and Geneticist improves therapy choices since the condition is rare.
Support
References
- Grigg C, Anderson D, Earnshaw J. Diagnosis and treatment of hereditary hemorrhagic telangiectasia. Ochsner Journal. 2017;17:157–161. Accessed March 25, 2021. https://www.ochsnerjournal.org/content/ochjnl/17/2/157.full.pdf
- Riera-Mestre A, Mora-Luján, J, Trujillo-Santos J, et al. RIETE Investigators. Natural history of patients with venous thromboembolism and hereditary hemorrhagic telangiectasia. Findings from the RIETE Registry. Orphanet J Rare Dis. 2019;14:196. doi:10.1186/s13023-019-1172-8. https://ojrd.biomedcentral.com/articles/10.1186/s13023-019-1172-8
- Jarzabek M, Trojanowski P, Szajner M, Pyra K, Sojka M, Szczerbo-Trojanowska M. Epistaxis in Rendu-Osler-Weber disease treated with selective embolization – case report. Przegl Lek. 2012;69(7):317-319. Accessed March 25, 2021. https://pubmed.ncbi.nlm.nih.gov/23276024/
- Kritharis A, Al-Samkari H, Kuter D. Hereditary hemorrhagic telangiectasia: Diagnosis and management from the hematologist’s perspective. Haematologica. 2018;103(9):1433-1443. doi:10.3324/haematol.2018.193003. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6119150/
- Inoguchi Y, Kaku B, Kitagawa N, Katsuda S. Hereditary hemorrhagic telangiectasia with SMAD4 mutations is associated with fatty degeneration of the left ventricle, coronary artery aneurysm, and abdominal aortic aneurysm. Intern Med. 2019;58(3):387-393. doi:10.2169/internalmedicine.1287-18. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC 6395134/h
6. Dittus C, Streiff M, Ansell J. Bleeding and clotting in hereditary hemorrhagic telangiectasia. World J Clin Cases. 2015;3(4):330-337. doi:10.12998/wjcc.v3.i4.330. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4391002/
7. Brinjikji W, Nasr D, Cloft H, Iyer V, Lanzino G. Spinal arteriovenous fistulae in patients with hereditary hemorrhagic telangiectasia: A case report and systematic review of the literature. Interv Neuroradiol. 2016;22(3):354-361. doi:10.1177/1591019915623560. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4984358/
8. Shovlin C. Hereditary haemorrhagic telangiectasia. Cancer Ther Advisor. Published 2017. Accessed March 25, 2021. https://www.cancertherapyadvisor.com/home/decision-support-in-medicine/hematology/hereditary-haemorrhagic-telangiectasia/
9. National Organization for Rare Disorders. Hereditary hemorrhagic telangiectasia. Published 2021. Accessed March 25, 2021. https://rarediseases.org/rare-diseases/hereditary-hemorrhagic-telangiectasia/
10. Weingarten T, Hanson J, Anusionwu K, et al. Management of patients with hereditary hemorrhagic telangiectasia undergoing general anesthesia: A cohort from a single academic center’s experience. J Anesth. 2013;27(5):705-711. doi:10.1007/s00540-013-1601-0. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4267556/
11. Devlin H, Hosman A, Silva B, Shovlin C. Evaluation of anticoagulant and antiplatelet use in haemorrhagic disorder. The Lancet. 2014;383:40. doi:10.1016/S0140-6736(14)60303-2. https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(14)60303-2/fulltext
12. Cure HHT. Diagnostic criteria for HHT. Published 2021. Accessed March 25, 2021. https://curehht.org/understanding-hht/diagnosis-treatment/diagnostic-criteria-hht/