What is pulmonary hypertension?
Pulmonary hypertension is a condition where the blood pressure in the pulmonary arteries (the vessels that carry blood from the heart to the lungs) is higher than normal. This puts a strain on the right side of the heart, which has to work harder to pump the blood through.
Pulmonary hypertension from all causes may affect up to 500 in every 100,000 people in Australia.
Pulmonary hypertension symptoms
In the early stages of pulmonary hypertension, there are often no symptoms or signs. When symptoms do appear, they often only occur with exercise, but later they may also occur at rest.
Symptoms of pulmonary hypertension may include:
- breathlessness;
- tiredness;
- fast heartbeat or palpitations (an awareness of your heart beating or pounding);
- fainting or feeling light-headed or dizzy;
- chest pain;
- cyanosis (a bluish discolouration of the skin, often appearing around your lips); and
- swelling of the legs and feet (oedema).
What causes it?
Pulmonary hypertension is associated with inflammation, stiffening and narrowing of the blood vessels that carry blood from the heart to the lungs. These changes to the pulmonary arteries mean that it is harder for the heart to pump blood through them – causing the blood pressure in the arteries to rise.
In rare cases, the cause of pulmonary hypertension is unknown. This is called idiopathic pulmonary arterial hypertension (PAH). Pulmonary hypertension can also be an inherited genetic condition (called familial pulmonary arterial hypertension).
In most cases, pulmonary hypertension is associated with another disease, such as:
- chronic obstructive lung disease (COPD), a long-term respiratory condition usually caused by smoking;
- interstitial lung diseases (lung conditions that involve scarring of the lung tissue, such as pulmonary fibrosis);
- connective tissue disorders, including scleroderma and lupus;
- blood clots in the lungs (pulmonary embolism);
- sleep apnoea;
- certain congenital (present from birth) heart defects;
- heart conditions that affect one of the valves in the left side of the heart (mitral valve disease or aortic valve disease);
- blood disorders such as sickle cell disease;
- certain chronic (ongoing) liver conditions; and
- HIV infection.
Pulmonary hypertension is also associated with some drugs and medicines, such as certain appetite suppressants (‘diet pills’), methamphetamine and cocaine.
Pulmonary hypertension has been classified into 5 groups according to the cause by the World Health Organization (WHO).
Complications
In some cases of pulmonary hypertension, the right side of the heart has to work very hard to pump blood against the resistance of the pulmonary arteries. This can eventually result in enlargement of the right side of the heart and right-sided heart failure.
Other complications include:
- blood clots in the blood vessels in the lungs;
- an irregular heartbeat (arrhythmia); and
- bleeding in the lungs.
How is pulmonary hypertension diagnosed?
Your doctor will ask about your symptoms, medical and family history, and check for signs of pulmonary hypertension.
If your doctor suspects that you may have pulmonary hypertension, they will usually refer you to a centre specialising in this disease for further investigation.
Tests
There are several tests that may be recommended to diagnose pulmonary hypertension. Tests may also be needed to determine how severe it is and the likely cause of the pulmonary hypertension.
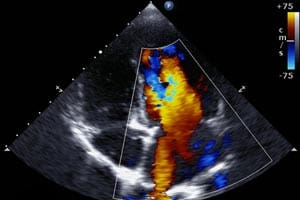
An echocardiogram is a type of ultrasound scan that can estimate the pressure in the pulmonary blood vessels, as well as determine the size of the heart and the blood vessels to the lungs. An echocardiogram can also show how the heart is functioning. If the results of an echocardiogram suggest a diagnosis of pulmonary hypertension, your doctor may recommend you have a test called a right heart catheterisation.
Right heart catheterisation is the best test for confirming the diagnosis of pulmonary hypertension and determining its severity. This involves threading a fine tube through one of your blood vessels (usually a blood vessel in the groin) up to the heart, where the pressure in the pulmonary arteries can be accurately measured.
Exercise tests may also be recommended to determine the severity of your condition. The severity of pulmonary hypertension is usually graded – the grading system is called the PAH functional class and relates to the severity of your symptoms at rest and during activity.
Other tests may be done to determine the cause of pulmonary hypertension and to check for any complications. These tests may include:
- lung function tests;
- chest X-ray;
- chest CT scan or MRI;
- tests for sleep-disordered breathing, including sleep apnoea (e.g. overnight sleep study – polysomnogram);
- electrocardiogram (ECG); and
- blood tests.
Pulmonary hypertension treatment
Unfortunately there is no cure for most types of pulmonary hypertension. However, there are treatments to help control symptoms and improve your quality of life.
Treatment will vary depending on the cause and severity (functional class) of your pulmonary hypertension.
Early diagnosis and treatment helps improve outcomes in people with pulmonary hypertension. Your doctor will most likely refer you to a specialist in respiratory medicine (called a respiratory physician) for treatment.
Medicines
Medicines are now available for the specific treatment of pulmonary hypertension. Medicines are usually prescribed by a specialist, and can help improve symptoms and quality of life.
Pulmonary vasodilator medicines open narrowed blood vessels and include:
- epoprostenol (brand names Flolan, Veletri);
- iloprost (Ventavis); and
- treprostinil (Remodulin).
Endothelin receptor antagonists are medicines that reverse the effect of endothelin, a substance in the walls of blood vessels that causes them to narrow. These medicines include:
- ambrisentan (brand name Volibris);
- bosentan (Tracleer); and
- macitentan (Opsumit).
Phosphodiesterase type 5 inhibitors (PDE-5 inhibitors) also work by opening blood vessels in the lungs. These medicines include:
- sildenafil (brand name Revatio); and
- tadalafil (Adcirca).
Selexipag (brand name Uptravi) is a medicine that also dilates blood vessels and can be used to treat pulmonary hypertension.
Other medicines used to treat pulmonary hypertension may include:
- anticoagulants (to reduce the risk of blood clots);
- diuretics (to remove excess fluid and so reduce the work of the heart); and
- calcium channel blocker medicines (to relax the blood vessels and so lower the blood pressure).
Other treatments
There are other treatments available for treating the symptoms of pulmonary hypertension, including the following.
- Some people may need oxygen therapy if their breathing gets worse.
- In people with pulmonary hypertension due to blood clots in the lungs, surgery to remove scar tissue in the pulmonary blood vessels may be an option.
- In very severe cases, if medical treatments are not working, a lung or heart-lung transplant may be considered.
Australian support groups
Talk to your doctor about support groups for people with pulmonary hypertension and their families.