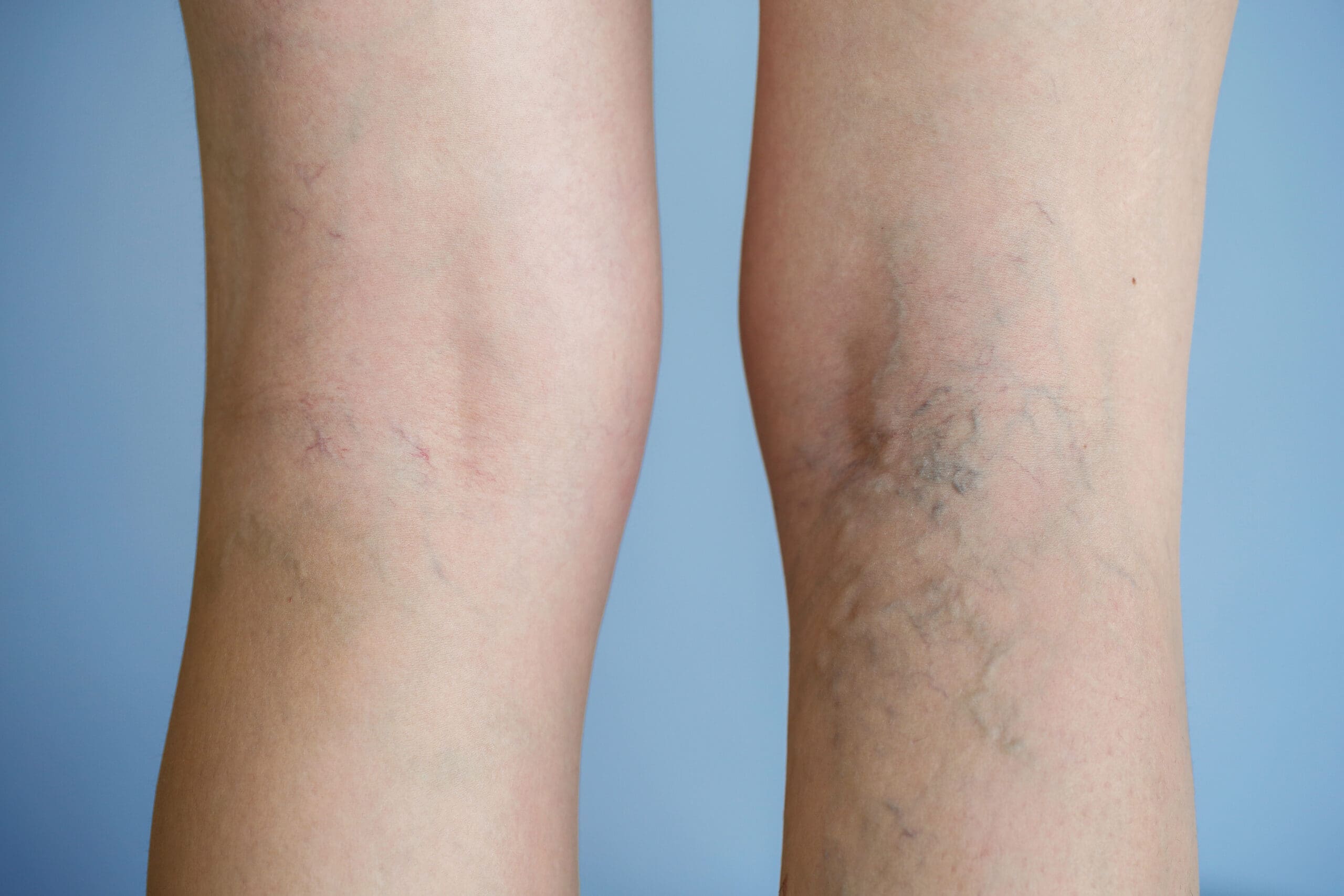
Varicose veins are veins that have become visibly twisted and swollen. They most commonly occur in the legs and feet.
While the only downside of varicose veins for some people is their appearance, other people have symptoms such as aching legs and skin irritation. They are not usually a major health concern, but some people do develop complications that can be serious.
There are several treatments that can fix varicose veins. The best treatment for you will depend on the extent of the problem and your personal preferences.
What are the symptoms of varicose veins?
Varicose veins are a cosmetic concern for many people, appearing as visible blue or purple veins under the skin or twisted, swollen veins that are like cords on the legs.
Initially, varicose veins are usually painless, but over time they can cause symptoms and signs such as:
- aching pain or heaviness in the legs, especially when standing and walking;
- cramps in the legs, most often at night;
- tired legs;
- mild swelling of the legs, ankles and feet;
- discoloured skin in the area around the varicose veins;
- an itchy rash (varicose eczema);
- burning of the skin over the veins; and
- restless legs.
Many people with varicose veins find that their symptoms are better in the morning. They also tend to improve when they put their feet up or walk around.
Spider veins (tiny red or blue veins that resemble a spider web) are a smaller, milder variation of varicose veins.
How do varicose veins develop?
Veins have the job of taking blood back to the heart. Blood moves from the superficial veins (found just under the skin) through perforator veins to the deep veins in the leg muscles.
Because the leg veins are working against gravity, they have one-way valves inside them to prevent the backflow of blood. Your leg muscles also help blood to flow the right way – when they are used, as in walking, they act as a pump, sending the blood in the veins up to the heart.
If the walls of leg veins lose their elasticity and weaken, the valves can stop functioning properly. This means that blood can flow backwards and pool in the veins, causing them to swell and become varicose. Varicose veins usually affect the superficial leg veins (the veins just under the skin).
Are varicose veins dangerous?
In general, varicose veins are not dangerous. However, some people experience significant discomfort associated with their varicose veins. Skin changes can also occur, including discolouration of the skin over the veins.
Occasionally, people with varicose veins develop ulcers on the legs, usually near the ankles. These ulcers can be extremely painful and take a long time to heal.
A blood clot and inflammation in the varicose veins is another possible complication. This is known as thrombophlebitis. Bleeding from varicose veins is another possible, but rare, complication.
What causes varicose veins?
The exact cause of varicose veins is not known. However, there seems to be a genetic link, meaning you are more likely to have them if one of your parents was affected.
It’s also thought that female sex hormones (oestrogen and progesterone) can sometimes play a part in veins becoming dilated (widened).
Having previously had a deep vein thrombosis (DVT) also seems to play a role in the development of varicose veins in some people. If you’ve had a blood clot in one of the deep veins of the legs, the valves in that vein may be damaged. This can increase the pressure in the superficial veins, causing widening and the development of varicose veins.
Risk factors
Factors that can increase your chances of developing varicose veins include:
- increasing age;
- pregnancy;
- family history of varicose veins;
- being overweight;
- being female; and
- standing still or sitting for long periods of time.
If you have a job where you are required to stand up most of the time your risk of developing varicose veins is higher. Previous injury to the legs can also increase your risk.
Diagnosis and tests
Doctors can often diagnose varicose veins by simply examining the veins in the legs. Your doctor will want to look at the veins in your legs when you are standing up, and examine the skin of your legs too.
Your doctor may recommend taking photos of the areas affected to track progress of the disease or to show improvements after treatment.
Your doctor may recommend having an ultrasound scan to look at the veins in your legs, check for blood clots and check whether the valves in the veins are functioning properly.
Treatment for varicose veins
Many people don’t need any specific treatment for varicose veins other than self-care measures. However, without treatment, varicose veins do tend to get worse with time. One exception to this is varicose veins that develop during pregnancy, which generally get better within several months of the birth.
The aim of treatment is to ease symptoms, improve appearance and prevent complications such as leg ulcers. Varicose veins can usually be successfully treated, but new varicose veins are still likely to develop over time.
These days there are several non-invasive or minimally-invasive treatment options for varicose veins. These can be done as outpatient procedures and don’t have a long recovery time, so are often recommended instead of surgery.
Talk to your doctor about treatment options and which type of treatment would be best for you. If necessary, your doctor will refer you to a specialist – several specialists offer treatments for varicose veins, including surgeons, dermatologists (skin specialists) and phlebologists (vein specialists).
Self-help for varicose veins
Several self-help measures can help treat the discomfort of varicose veins and stop them from getting worse. These include:
- regular exercise that improves the muscle tone in your legs;
- losing weight if you are overweight;
- avoiding clothes that are tight around the legs, groin and waist;
- keeping your legs elevated when you are sitting; and
- avoiding standing still for prolonged periods.
Wearing flat shoes may help work your calf muscles and improve the circulation in your legs.
Compression stockings
Wearing elasticised compression stockings is often suggested by doctors as the initial treatment for varicose veins. These stockings create gentle pressure up the leg to prevent blood from pooling in the veins. They can help with leg pain and swelling.
The stockings are available on prescription or over the counter, but work best when properly fitted. They should be worn all day for best effect. You don’t need to wear them overnight while you are sleeping.
Your doctor may also recommend you wear compression stockings after other treatments for varicose veins to stop them coming back.
Endovenous thermal ablation
This treatment involves destroying varicose veins using endovenous laser ablation (EVLA) or radiofrequency ablation (RFA).
It involves inserting a catheter (a very thin, hollow tube) into the varicose veins, under ultrasound guidance to make sure it is in the right place. Radiofrequency or laser energy is then applied via the tip of the catheter along the inside of the vein, heating it up and causing the walls to collapse and close together. The vein is replaced by scar tissue and eventually removed by the body.
This treatment can be used for spider veins as well as varicose veins, with reported success rates of around 95 per cent.
Injection sclerotherapy
Sclerotherapy is a form of treatment that involves injecting varicose veins with a chemical solution that irritates and scars the vessel walls, making them stick together. This blocks off the veins, which are replaced by scar tissue and then removed by the body’s immune system.
Sclerotherapy is usually effective when used to treat spider veins and small varicose veins. It may need to be repeated several times. A newer sclerotherapy technique – foam sclerotherapy – involves injecting foam sclerosant, usually under ultrasound guidance. Foam sclerotherapy may be more effective in treating larger varicose veins.
Specially-fitted compression stockings must be worn day and night for several weeks after sclerotherapy to ensure that the vein walls stick together and form scar tissue.
Surgery
Surgery for varicose veins can be very effective and usually leaves little in the way of scars.
Ambulatory phlebectomy is usually used for small veins that are close to the skin surface. It involves removing varicose veins in the lower leg through a series of tiny skin punctures.
Vein stripping and ligation is where longer veins are tied shut and removed through small cuts in the skin. This type of surgery is usually used to treat more severe cases of varicose veins.
Which treatment is best?
If you have varicose veins, ask your doctor about the most appropriate type of treatment for you. In general, it will depend on where your varicose veins are and how extensive they are. Treatments aim to either close off the varicose veins or remove them.
Also ask about the side effects of different treatments. Common short-term side effects of many treatments for varicose veins include swelling, bruising and mild pain. Infection is also a risk.
Can you prevent varicose veins?
There are several steps you can take to help reduce your risk of developing varicose veins. These include avoiding prolonged standing or sitting, losing weight if you are overweight and exercising. Putting your legs up when you are sitting may also be a good idea.
If you already have an increased risk, for example if you have a family history of varicose veins, you may want to consider wearing graduated compression stockings.
People who have been treated for varicose veins should continue to avoid prolonged standing and wear graduated compression stockings if they will be standing for any period of time.