insulin detemir (rys)
Consumer Medicine Information
What is in this leaflet
What Levemir® is used for
Before you use Levemir® FlexPen®
How to use Levemir® FlexPen®
While you are using Levemir® FlexPen®
Side effects
After using Levemir® FlexPen®
Product description
Further information
Instructions for Use
This leaflet answers some common questions about Levemir® FlexPen®. It does not contain all the available information. It does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor has weighed the risks of you using Levemir® FlexPen® against the benefits they expect it will have for you.
If you have any concerns about using this medicine, ask your doctor, diabetes education nurse or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
What Levemir® is used for
The insulin detemir (rys), or “Levemir®”, in Levemir® FlexPen® is a long-acting insulin used to treat diabetes mellitus. It may be used in combination with oral antidiabetic medicines (diabetes tablets) or as add-on therapy to liraglutide (Victoza®), which is used to treat type 2 diabetes mellitus in adults. Levemir® can also be used with a meal-related short- or rapid-acting insulin such as NovoRapid®.
Diabetes mellitus is a condition where your pancreas does not produce enough insulin to control your blood sugar (glucose) level. Extra insulin is therefore needed.
There are two types of diabetes mellitus:
Type 1 diabetes – also called juvenile onset diabetes
Type 2 diabetes – also called maturity onset diabetes.
Patients with type 1 diabetes always require insulin to control their blood sugar levels.
Some patients with type 2 diabetes may also require insulin after initial treatment with diet, exercise and tablets.
Levemir® lowers your blood sugar level after injection. The effect may last for up to 24 hours.
As with all insulins, the duration of action will vary according to the dose, injection site, blood flow, temperature and level of physical activity.
FlexPen® is a pre-filled dial-a-dose insulin pen able to deliver from 1 to 60 units of Levemir® in increments of 1 unit.
This medicine is not addictive.
Levemir® FlexPen® is available only with a doctor’s prescription.
Ask your doctor, diabetes education nurse or pharmacist if you have any questions about why this medicine has been prescribed for you.
Before you use Levemir® FlexPen®
When you must not use it
Do not use this medicine if:
- you have an allergy to:
- any medicine containing insulin
- any of the ingredients listed in the ‘Ingredients’ section of this leaflet.
Some of the symptoms of an allergic reaction may include:
– redness, swelling, rash and itching at the injection site
– rash, itching or hives on the skin
– shortness of breath
– wheezing or difficulty breathing
– swelling of the face, lips, tongue or other parts of the body.
- you are experiencing low blood sugar levels (a “hypo”) when your dose is due.
If you have a lot of hypos discuss appropriate treatment with your doctor.
If you are not sure whether you should start using this medicine, talk to your doctor.
Do not use this medicine after the expiry date printed on the pack, or if the packaging is torn or shows signs of tampering. If it has expired or is damaged, return it to your pharmacist for disposal.
Before you start to use it
Tell your doctor if you have allergies to any other medicines, foods, preservatives or dyes.
Tell your doctor if you have or have had any of the following medical conditions:
- kidney problems
- liver problems
- adrenal, pituitary or thyroid gland problems.
Tell your doctor if you are pregnant or plan to become pregnant. Pregnancy may make managing your diabetes more difficult. Insulin needs usually decrease during the first three months of pregnancy and increase during the last six months. Your doctor can discuss with you the risks and benefits involved.
Tell your doctor if you are breast-feeding or plan to breast-feed. Your doctor can discuss with you the risks and benefits involved.
Inform your doctor as soon as possible if you experience signs of heart failure such as unusual shortness of breath or rapid increase in weight or localised swelling (oedema). Some patients with long-standing type 2 diabetes mellitus and heart disease or previous stroke who are treated with thiazolidinediones in combination with insulin may develop heart failure.
If you have not told your doctor about any of the above, tell them before you start using this medicine.
Tell your doctor if you notice any skin changes at the injection site. The injection site should be rotated to help prevent changes to the fatty tissue under the skin, such as skin thickening, skin shrinking or lumps under the skin. The insulin may not work very well if you inject into a lumpy, shrunken or thickened area (see How to use Levemir® FlexPen®). Tell your doctor if you notice any skin changes at the injection site. Tell your doctor if you are currently injecting into these affected areas before you start injecting in a different area. Your doctor may tell you to check your blood sugar more closely, and to adjust your insulin or your other antidiabetic medications dose.
Taking other medicines
Tell your doctor if you are taking any other medicines, including any that you get without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and Levemir® may interfere with each other and this may mean that your insulin dose has to change.
If you take any of the medicines listed below, your blood sugar level may fall (hypoglycaemia):
- other medicines used for the treatment of diabetes
- monoamine oxidase inhibitors (MAOI) – used for the treatment of depression
- alpha blockers – used to treat high blood pressure and to relieve difficulty in passing urine caused by an enlarged prostate
- non-selective beta blockers – used to treat high blood pressure and certain heart conditions which may also mask the symptoms of hypoglycaemia and delay recovery from hypoglycaemia
- ACE inhibitors – used to treat high blood pressure, certain heart conditions or elevated protein/albumin in the urine
- salicylates e.g. aspirin – used to relieve pain and lower fever
- anabolic steroids – used to promote growth
- sulphonamides – used to treat bacterial infections
- quinine – used to treat malaria and relieve muscle cramps
- quinidine – used to treat heart problems.
If you take any of the medicines below, your blood sugar level may rise (hyperglycaemia):
- glucocorticoids (except when applied locally) – used to treat inflammatory conditions
- oral contraceptives (“the pill”) – used for birth control
- diuretics e.g. thiazides, frusemide or ethacrynic acid – used to treat high blood pressure or fluid retention (oedema)
- thyroid hormones – used to treat malfunction of the thyroid gland
- sympathomimetics – used to treat asthma
- growth hormone – used to treat growth disorders.
- danazol – used to treat endometriosis, menorrhagia, fibrocystic breast disease and hereditary angioedema
- oxymetholone – used to treat certain blood disorders
- diazoxide – used to treat high blood pressure
- nicotinic acid – used to treat high cholesterol levels in the blood
- asparaginase – used to treat leukaemia and lymph gland tumours.
If you take the following medicines, your blood sugar level may rise or fall:
- octreotide – used to treat gastrointestinal endocrine tumours and enlargement of parts of the body (e.g. hands, feet, head) caused by abnormal growth hormone levels
- lanreotide – used to treat enlargement of parts of the body (e.g. hands, feet, head) caused by abnormal hormone levels.
Tell your doctor about any other medicines that you are taking. This is very important. Your doctor will advise you if it is alright to keep taking them or if you should stop taking them.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while using this medicine.
How to use Levemir® FlexPen®
Your doctor, diabetes education nurse or pharmacist will have given you advice on how to use your medicine. Carefully follow all the directions. They may differ from the information contained in this leaflet.
Any change in dose or type of insulin should be made cautiously and only under medical supervision. If you change the type of insulin that you use, you may have to use more or less than before. This may happen with the first dose or over a period of time.
If you do not understand the instructions, ask your doctor, diabetes education nurse or pharmacist for help.
How much to use
Your doctor or diabetes education nurse will tell you how much of this medicine you need to use.
It is very important that you manage your diabetes carefully. Too much or too little insulin can cause serious effects.
When to use it
Levemir® is either injected once or twice daily. If you require twice daily dosing, the evening dose can be administered either with the evening meal, at bedtime, or 12 hours after the morning dose. Your doctor will tell you when to inject your medicine.
How to use it
- Inject Levemir® under the skin (subcutaneous injection) as shown to you by your doctor or diabetes education nurse. Never inject Levemir® directly into a vein or muscle.
- Levemir® may be injected into your abdomen, thigh, buttock or upper arm.
- Remember to change your injection site regularly as shown to you by your doctor or diabetes education nurse. This reduces the risk of developing lumps or skin pitting.
- Do not use Levemir® in insulin pumps.
Checking your Levemir® FlexPen®:
Check your medicine before each preparation and injection. Make sure you are using the correct type of insulin.
Levemir® is a clear colourless solution. Do not use this medicine if it is thickened, coloured, or has solid bits in it.
Read the instructions printed later in this leaflet carefully in order to prepare and handle your Levemir® FlexPen® correctly.
How long to use it
Do not stop using Levemir® FlexPen® unless your doctor tells you to.
If you use too much (overdose) – Hypoglycaemia
Your blood sugar level may become too low (you may experience hypoglycaemia or a “hypo”) if you:
- use too much insulin
- miss a meal
- exercise more than usual
- are ill.
The first symptoms of mild to moderate hypos can come on suddenly. They may include:
- cold sweat, cool pale skin
- fatigue, drowsiness, unusual tiredness and weakness
- nervousness, anxious feeling, tremor, rapid heart beat
- confusion, difficulty concentrating
- excessive hunger
- vision changes
- headache, nausea.
Always carry some sugary food or fruit juice with you. If you experience any of these symptoms of a hypo, immediately eat some sugary food or have a sugary drink, e.g. lollies, biscuits or fruit juice, and measure your blood sugar level.
Tell your relatives, friends, close workmates or carers that you have diabetes. It is important that they recognise the signs and symptoms of a hypo.
Make sure they know to give you some sugary food or fruit juice for mild to moderate symptoms of a hypo.
If you lose consciousness, make sure they know:
- to turn you on your side and get medical help immediately
- not to give you anything to eat or drink.
This is because you could choke.
An injection of the hormone glucagon may speed up recovery from unconsciousness. This can be given by a relative, friend, workmate or carer who knows how to give it.
If glucagon is used, eat some sugary food or have a sugary drink as soon as you are conscious again.
If you do not feel better after this, contact your doctor, diabetes education nurse, or the closest hospital.
If you do not respond to glucagon treatment, you will have to be treated in a hospital.
See your doctor if you keep having hypo reactions, or if you have ever become unconscious after using insulin. The amount or timing of insulin, food or exercise may need to be adjusted.
If a prolonged, severe hypo is not treated it can cause brain damage and death.
If you miss a dose – Hyperglycaemia
If you forget your insulin dose, check your blood sugar level and test your urine for ketones as soon as possible.
If you are not sure what to do, talk to your doctor, diabetes education nurse or pharmacist.
Do not use a double dose of your insulin. If it is almost time for your next dose, skip the dose you missed and use your next dose when you are meant to.
Otherwise, use it as soon as you remember, and then go back to using it as you would normally.
Your blood sugar levels may become high (hyperglycaemia) if you:
- miss doses of insulin or use less insulin than you need
- have uncontrolled diabetes
- exercise less than usual
- eat more carbohydrates than usual
- are ill or stressed.
High blood sugar levels over a long period of time can lead to too much acid in the blood (diabetic ketoacidosis).
Contact your doctor immediately if your blood sugar level is high or you recognise any of the following symptoms.
Symptoms of mild to moderate hyperglycaemia include:
- drowsy feeling
- flushed face
- thirst, loss of appetite
- fruity odour on the breath, dry mouth
- blurred vision
- passing larger amounts of urine than usual
- getting up at night more often than usual to pass urine
- high levels of glucose and acetone in the urine.
Symptoms of severe hyperglycaemia include:
- heavy breathing
- fast pulse
- nausea, vomiting
- dehydration
- loss of consciousness.
Severe hyperglycaemia can lead to unconsciousness and in extreme cases death if untreated.
Discuss any worries you may have about this with your doctor, diabetes education nurse or pharmacist.
While you are using Levemir® FlexPen®
Things you must do
Measure your blood sugar level regularly.
Make sure all friends, relatives, workmates and carers know that you have diabetes and are using insulin. If your child has diabetes it is important to tell their carers.
Keep using your insulin even if you feel well. It helps to control your condition, but does not cure it.
Tell your doctor if you often have hypos (low blood sugar levels). Your doctor may need to adjust your insulin dose.
Always carry some sugary food or fruit juice with you. If you experience any of the symptoms of a hypo, immediately eat some sugary food or have a drink, e.g. lollies, biscuits or fruit juice, and measure your blood sugar level.
Tell your doctor if you have trouble recognising the symptoms of hypos. Under certain conditions, the early warning signs of hypos can be different or less obvious. Your doctor may need to adjust your insulin dose.
Make sure that you tell every doctor, dentist, pharmacist or other health care professional who is treating you that you have diabetes and are using insulin.
Tell your doctor, diabetes education nurse or pharmacist if you are travelling. Ask them for a letter explaining why you are taking injecting devices with you. Each country you visit will need to see this letter, so you should take several copies.
You may need to inject your insulin and eat your meals at different times because of time differences in and between countries.
You may not be able to get the same type of insulin in the country you are visiting.
Your doctor, diabetes education nurse or pharmacist can provide you with some helpful information.
Things you must not do
Do not stop using Levemir® FlexPen® unless your doctor tells you to.
Do not use this medicine if you think it has been frozen or exposed to excessive heat. It will not work as well.
Do not use this medicine to treat any other complaints unless your doctor tells you to.
Do not give your medicine to anyone else, even if they have the same condition as you.
Do not share needles.
Things to be careful of
Be careful driving or operating machinery until you know how the insulin affects you.
If your blood sugar is low or high your concentration and ability to react might be affected and therefore also your ability to drive or operate a machine. Bear in mind that you could endanger yourself or others. Please ask your doctor whether you can drive a car:
- if you have frequent hypos
- if you find it hard to recognise hypos.
Tell your doctor if you drink alcohol. Alcohol may mask the symptoms of hypos. If you are drinking alcohol your need for insulin may change, as your blood sugar level may either rise or fall. Careful monitoring is recommended.
Tell your doctor if you are ill. Illness, especially with nausea and vomiting, may cause your insulin needs to change. Even if you are not eating, you still require insulin. You and your doctor should design an insulin plan for those times when you are sick.
Tell your doctor if you are exercising more than usual. Exercise may lower your need for this medicine. Exercise may also speed up the effect of a dose of it, especially if the exercise involves the area of the injection site (e.g. the leg should not be used for injection prior to jogging or running).
Tell your doctor if your diet changes. Insulin is essential to keep your blood sugar levels within acceptable limits. Regular meals and a balanced diet are important factors in the management of diabetes. It is important that you discuss a suitable diet plan with your doctor or diabetes team.
Smoking may increase the chance of complications with your diabetes.
Side effects
Tell your doctor, diabetes education nurse or pharmacist as soon as possible if you do not feel well while you are using Levemir® FlexPen®.
This medicine helps most people for whom it is prescribed, but it may have unwanted side effects in a few people. All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical treatment if you get some of the side effects.
Do not be alarmed by the following lists of side effects. You may not experience any of them.
Ask your doctor, diabetes education nurse or pharmacist to answer any questions you may have.
The most common side effect when using insulin is low blood sugar levels (a hypo).
Tell your doctor if you notice any of the following and they worry you:
- hypos (mild to moderate)
- pain, redness, swelling, hives, inflammation, bruising or itching at the injection site. Usually these symptoms disappear within a few weeks during continued use. If you have serious or continuing reactions, you may need to stop using Levemir® and use another insulin.
- a depression or thickening of the skin around the injection site (lipodystrophy). If you inject insulin at the same place, the fatty tissue may shrink (lipoatrophy) or thicken (lipohypertrophy). Lumps under the skin may also be caused by build-up of a protein called amyloid (cutaneous amyloidosis; how often this occurs is not known). The insulin may not work very well if you inject into a lumpy, shrunken or thickened area. Change the injection site with each injection to help prevent these skin changes.
- when you first start your insulin treatment you may get visual problems or swollen hands and feet.
This list includes the more common side effects of your medicine. They are usually mild and short-lived.
If any of the following happen, tell your doctor immediately or go to Accident and Emergency at your nearest hospital:
More severe symptoms of low blood sugar levels, including:
- disorientation
- seizures, fits or convulsions
- loss of consciousness.
If a severe hypo is not treated, it can cause brain damage and death.
Tell your doctor immediately or go to Accident and Emergency at your nearest hospital if you notice any of the following:
- skin rashes over a large part of the body
- shortness of breath, wheezing
- swelling of the face, lips or tongue
- fast pulse
- sweating.
This list includes very serious side effects. You may need urgent medical attention or hospitalisation. These side effects are very rare.
Tell your doctor if you notice anything that is making you feel unwell.
Other side effects not listed above may also occur in some people.
Ask your doctor, diabetes education nurse or pharmacist to answer any questions you have.
After using Levemir® FlexPen®
Storage
Before opening:
Store Levemir® FlexPen® that are not being used between 2°C and 8°C in a refrigerator (not in or too near the freezer section or cooling element).
During use or when carried as a spare:
Store Levemir® FlexPen® that you are using, or that you are carrying as a spare up to 4 weeks below 30°C or between 2°C and 8°C in a refrigerator.
Discard Levemir® FlexPen® after 4 weeks even if there is still some medicine left in it.
The Levemir® in Levemir® FlexPen® must not be frozen, or exposed to excessive heat or light. Protect the medicine in Levemir® FlexPen® from light by keeping the pen cap on when not in use.
Do not use Levemir® after the expiry date which is stated on the FlexPen® label and carton after ‘Expiry’.
Never use Levemir® FlexPen® if the solution is not clear and colourless.
Keep out of the reach of children.
Disposal
Dispose of used needles safely into a sharps container.
If your doctor tells you to stop using this medicine or the expiry date has passed, ask your pharmacist what to do with any medicine that is left over.
Product description
What it looks like
Levemir® is a clear, colourless, aqueous solution for subcutaneous injection. Levemir® FlexPen® is a 3mL pre-filled glass cartridge contained in a dial-a-dose insulin pen.
Ingredients
Levemir® contains insulin detemir (rys) 100 units per mL (100 U/mL) as the active ingredient. The abbreviation “rys” indicates the method of genetic engineering used to manufacture this insulin.
Levemir® also contains the following inactive ingredients:
- glycerol
- phenol
- metacresol
- zinc acetate
- sodium chloride
- dibasic sodium phosphate dihydrate
- sodium hydroxide
- hydrochloric acid
- water for injections
Sponsor
Levemir® FlexPen® is supplied in Australia by:
Novo Nordisk Pharmaceuticals Pty. Ltd.
Level 10, 118 Mount Street,
North Sydney, NSW 2060
Levemir® FlexPen® is supplied in New Zealand by:
Novo Nordisk Pharmaceuticals Ltd.
11-19 Customs Street West,
Commercial Bay Tower,
Level 18, Office 1834,
Auckland 1010
This leaflet was prepared in October 2023.
Australian Registration Number: AUST R 172234
Levemir®, FlexPen®, NovoRapid®, Victoza®, NovoFine® and NovoCare® are registered trademarks of Novo Nordisk A/S.
© 2023
Novo Nordisk A/S
Further information
For further information call the NovoCare® Customer Care Centre on 1800 668 626 (Australia) or 0800 733 737 (NZ).
www.novonordisk.com.au
www.novonordisk.co.nz
You can also get more information about diabetes and insulin from Diabetes Australia and Diabetes New Zealand:
- freecall helpline 1300 136 588 (Australia)
- www.diabetesaustralia.com.au
- www.diabetes.org.nz
Instructions for Use
Introduction
Please read the following instructions carefully before using your FlexPen®. If you do not follow the instructions carefully, you may get too little or too much insulin, which can lead to too high or too low blood sugar levels.
Your FlexPen® is a pre-filled dial-a-dose insulin pen. You can select doses from 1 to 60 units in increments of 1 unit. FlexPen® is designed to be used with NovoFine® disposable needles up to a length of 8mm.
As a precautionary measure, always carry a spare insulin delivery device in case your FlexPen® in use is lost or damaged.
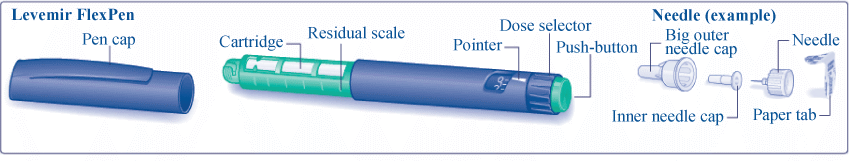
Caring for your pen
Your FlexPen® must be handled with care. If it is dropped, damaged or crushed, there is a risk of insulin leakage. This may cause inaccurate dosing, which can lead to too high or too low blood sugar levels.
You can clean the exterior of your FlexPen® by wiping it with an alcohol swab. Do not soak it, wash or lubricate it as it may damage the pen.
Do not refill your FlexPen®.
Preparing your Levemir® FlexPen®
Check the name and coloured label of your pen to make sure that it contains the correct type of insulin. This is especially important if you take more than one type of insulin. If you take the wrong type of insulin, your blood sugar level may get too high or too low.
A
Pull off the pen cap.

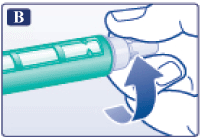
B
Remove the paper tab from a new disposable needle.
Screw the needle straight and tightly onto your FlexPen®.
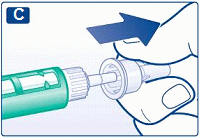
C
Pull off the big outer needle cap and keep it for later.
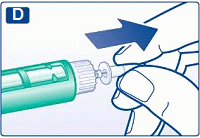
D
Pull off the inner needle cap and dispose of it.
Never try to put the inner needle cap back on the needle. You may stick yourself with the needle.
- Always use a new needle for each injection. This reduces the risk of contamination, infection, leakage of insulin, blocked needles and inaccurate dosing.
- Be careful not to bend or damage the needle before use.
Checking the insulin flow
Prior to each injection, small amounts of air may collect in the cartridge during normal use. To avoid injection of air and ensure proper dosing:
E
Turn the dose selector to select 2 units.
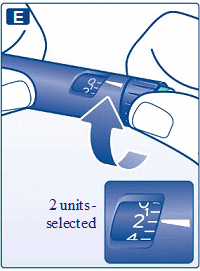
F
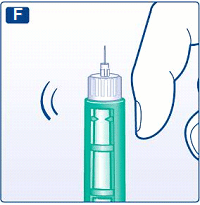
Hold your FlexPen® with the needle pointing upwards and tap the cartridge gently with your finger a few times to make any air bubbles collect at the top of the cartridge.
G
Keeping the needle upwards, press the push-button all the way in. The dose selector returns to 0.
A drop of insulin should appear at the needle tip. If not, change the needle and repeat the procedure no more than 6 times.
If a drop of insulin still does not appear, the pen is defective, and you must use a new one.

- Always make sure that a drop appears at the needle tip before you inject. This makes sure that the insulin flows. If no drop appears, you will not inject any insulin, even though the dose selector may move. This may indicate a blocked or damaged needle.
- Always check the flow before you inject. If you do not check the flow, you may get too little insulin or no insulin at all. This may lead to too high blood sugar levels.
Selecting your dose
Check that the dose selector is set at 0.
H
Turn the dose selector to select the number of units you need to inject.
The dose can be corrected either up or down by turning the dose selector in either direction until the correct dose lines up with the pointer. When turning the dose selector, be careful not to push the push-button as insulin will come out.
You cannot select a dose larger than the number of units left in the cartridge.

- Always use the dose selector and the pointer to see how many units you have selected before injecting the insulin.
- Do not count the pen clicks. If you select and inject the wrong dose, your blood sugar levels may get too high or too low. Do not use the residual scale, it only shows approximately how much insulin is left in your pen.
Making the injection
Insert the needle into your skin. Use the injection technique shown by your doctor or nurse.
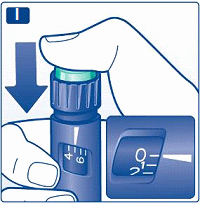
I
Inject the dose by pressing the push-button all the way in until 0 lines up with the pointer. Be careful only to push the push-button when injecting.
Turning the dose selector will not inject insulin.
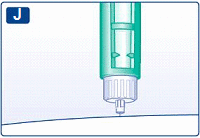
J
Keep the push-button fully depressed and let the needle remain under the skin for at least 6 seconds. This will make sure you get the full dose.
Withdraw the needle from the skin then release the pressure on the push-button.
Always make sure that the dose selector returns to 0 after the injection. If the dose selector stops before it returns to 0, the full dose has not been delivered, which may result in too high blood sugar levels.
K
Lead the needle into the big outer needle cap without touching it. When the needle is covered, carefully push the big outer needle cap completely on and then unscrew the needle.
Dispose of it carefully and put the pen cap back on.
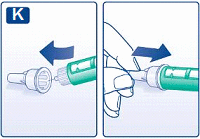
- Always remove the needle after each injection and store your FlexPen® without the needle attached. This reduces the risk of contamination, infection, leakage of insulin, blocked needles and inaccurate dosing.
Further important information
- Caregivers must be very careful when handling used needles – to reduce the risk of needle sticks and cross-infection.
- Dispose of your used FlexPen® carefully, without the needle attached.
- Never share your pen or your needles with other people. It might lead to cross-infection.
- Never share your pen with other people. Your medicine might be harmful to their health.
- Always keep your pen and needles out of sight and reach of others, especially children.
Published by MIMS January 2024
