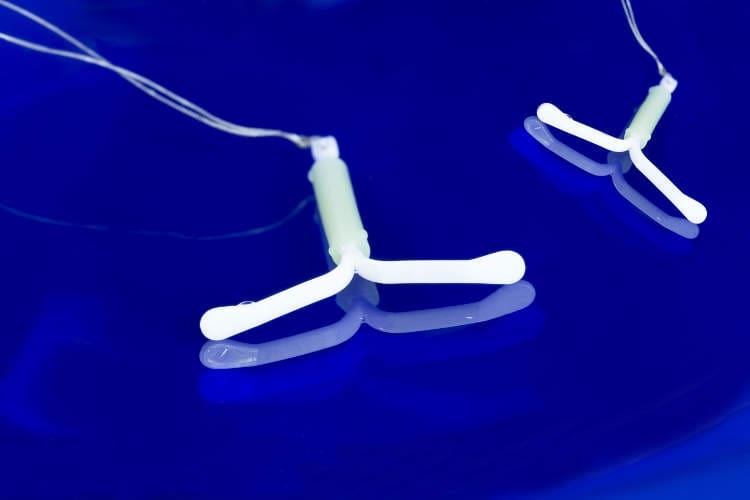
An intrauterine device (IUD) is a contraceptive device that is inserted into the uterus (womb) to stop you getting pregnant. IUDs are very reliable, safe and suitable for women of all ages. They can be used in women who want to have children in the future as well as in those who do not wish to have any future pregnancies.
IUDs provide effective contraception for at least 5 years, but can be taken out at any time if you no longer want to use contraception.
How do IUDs work?
IUDs are small, T-shaped devices made mostly of plastic with a nylon thread attached for easy removal. There are 2 types available in Australia – copper IUDs and hormonal IUDs.
Copper IUDs
Copper IUDs have copper wire bound around the vertical plastic stem. Examples of copper IUDs available in Australia include Load 375 Intrauterine device, TT380 Short Intrauterine device and TT380 Standard Intrauterine device. Depending on the brand used, copper IUDs can provide effective contraception for 5 to 10 years.
Copper IUDs work by changing conditions in the uterus, which affects the movement of sperm and eggs and reduces their viability. Copper IUDs also change the lining of the uterus, making it less suitable for a pregnancy.
Hormonal IUDs
Hormonal IUDs slowly release progestogen (a synthetic hormone that mimics the natural female sex hormone progesterone) into the body. The only hormonal IUD currently available in Australia is Mirena, which contains the progestogen levonorgestrel. Mirena provides effective contraception for 5 years.
Mirena works by thickening cervical mucus (mucus made made in the cervix – the lower part of the uterus). This prevents sperm from entering the uterus so that an egg cannot be fertilised.
Mirena also changes the lining of the uterus, making it less suitable for a pregnancy. In some women, it also stops ovulation (the release of an egg from the ovaries).
How effective are IUDs?
IUDs are more than 99 per cent effective in preventing pregnancy. So, less than one woman in every 100 using an IUD will become pregnant in a year. Levonorgestrel-releasing IUDs are slightly more reliable than copper IUDs.
Advantages
The advantages of using IUDs for contraception are that they:
- are very effective at preventing pregnancy;
- allow fertility to return immediately upon removal;
- don’t interfere with sexual spontaneity;
- can be used while breast feeding;
- are a long-term option for contraception (they work for 5 to 10 years);
- are relatively inexpensive; and
- require minimal ongoing attention.
An additional advantage of Mirena is that it can help reduce heavy menstrual bleeding (periods). In fact, many women experience no vaginal bleeding after 12 months of using Mirena.
Disadvantages
The disadvantages of using IUDs for contraception is that they:
- do not protect against sexually transmitted infections (STIs);
- need to be inserted by a trained health professional;
- may be difficult to insert in women who have not given birth vaginally;
- can increase the risk of pelvic infection for a few weeks after insertion; and
- may be expelled (fall out) undetected
- are not compatible with menstrual cups.
IUDs are not an option for all women. Hormonal IUDs are not suitable for women who have had breast cancer in the last 5 years. The risks of hormonal IUDs may also outweigh the benefits in women with liver disease, unexplained vaginal bleeding, heart disease, stroke or blood clots.
Women with a history of recurrent pelvic inflammatory disease or an ectopic pregnancy should discuss with their doctor the suitability of using any type of IUD.
Where can you get an IUD?
You will need to see your doctor or visit your local Family Planning Clinic to get an IUD. Your doctor will want to talk to you about the risks and benefits of IUDs and whether they would be a suitable option for you before prescribing an IUD and organising for it to be fitted (inserted).
IUDs need to be inserted by a specially trained doctor or nurse. GPs (general practitioners), doctors and nurses at Family Planning Clinics and gynaecologists (specialists in conditions affecting women’s reproductive organs) can insert IUDs. You will need a referral from your GP to see a gynaecologist.
How much does it cost to get an IUD?
Mirena is covered for most women in Australia on the PBS (Pharmaceutical Benefits Scheme), and usually costs around $40. It is cheaper if you have a Health Care Card – about $7. If you don’t have a Medicare card, they may cost up to $250 on private prescription.
Copper IUDs are not available on the PBS as they are devices, not medicines. Copper IUDs generally cost around $70 to $150.
The cost of the appointment to have the IUD inserted will vary depending on the doctor or clinic you go to. You can claim at least some of the cost of the IUD insertion appointment on Medicare.
When considering the cost of an IUD, bear in mind that it should last for 5 to 10 years.
Before you get an IUD
Your doctor will want to make sure that you are definitely not pregnant before inserting an IUD.
Your doctor will also want to check that you don’t have a sexually transmitted infection (STI) before inserting a new IUD or changing your IUD.
If your are at high risk of an STI, your doctor may recommend testing for an STI before inserting your device. This is important, because if there is an infection, inserting an IUD can increase the risk of pelvic inflammatory disease. Your doctor will recommend that you use condoms in addition to your IUD if you are at increased risk of STIs.
IUD insertion
Insertion is usually recommended during the first 7 days of your menstrual cycle (during your period or just after your period ends).
Some women experience a small amount of pain or discomfort during and after insertion, so your doctor may recommend you take painkillers (such as ibuprofen or paracetamol) about an hour before your appointment.
Inserting an IUD takes about 15 minutes. Your doctor will use a speculum (the same instrument used when you have a cervical cancer screening test – formerly a Pap smear) so that they can see your cervix. They may apply a local anaesthetic to your cervix before gently inserting the IUD using a special inserter device.
IUDs have a thread attached that comes through the cervix and sits high up in the vagina. You should be able to feel the thread if you put a finger high up into the vagina. It’s recommended that women regularly feel for the thread to make sure that the IUD is still in place. You should aim to do this about once a month.
It’s recommended that you avoid vaginal sex, using tampons, swimming and having baths for at least 2 days following the insertion of the IUD.
Removing IUDs
Depending on the type and brand of IUD you have, it needs to be replaced every 5 to 10 years to provide ongoing contraception.
An intrauterine device should be removed by a specially trained doctor or nurse. As with insertion, a speculum will be used to view your cervix and some local anaesthetic may be applied. Your doctor will remove the IUD by using instruments to locate and gently pull on the nylon string that is attached to the device. There may be some discomfort when the IUD is removed, but there should not be any lasting pain.
A new IUD can be inserted straight after the old one is removed if you want to continue to use an IUD for contraception.
Remember that you can have an IUD removed at any time if you want to become pregnant or you no longer wish to use an IUD. Your fertility should return to normal once the IUD is removed. That means that it’s possible to get pregnant as soon as the IUD is removed.
Side effects of IUDs
Most women with intrauterine devices have few side effects and find them to be an easy, set-and-forget method of contraception. However, as with any medicine or device, there are some possible side effects.
For a few days after the insertion of an IUD, you may experience some cramping, pelvic pain and vaginal bleeding. Cramping is usually more noticeable in women who have never given birth vaginally.
Copper IUDs
For a few weeks after being inserted, you may have irregular bleeding or spotting between periods. Copper intrauterine devices may cause periods to be heavier, longer and more painful than before.
Hormonal IUD
Possible side effects associated with use of Mirena include:
- erratic bleeding and spotting (this usually settles after the first 3 to 5 months after insertion);
- breast tenderness;
- acne;
- weight gain;
- headaches;
- nausea; and
- mood changes.
These side effects are more common immediately after insertion, and usually improve over time.
Risks of IUDs
Rarely, intrauterine devices can perforate (break through the wall of) the uterus. This risk of an IUD perforating the uterus appears to be higher in women who are breast feeding compared to women who are not breast feeding.
If a woman develops a pelvic infection while they have an IUD in place, antibiotics will be prescribed. If the infection persists despite the use of antibiotics, your doctor may recommend removing the IUD.
If a pregnancy should occur (which is rare), there is an increased risk that it will be in the fallopian tubes (ectopic pregnancy).
Your doctor can talk to you about the risks and benefits of IUDs to help you decide whether this may be a suitable form of contraception for you.
Check-ups when using an IUD
Your doctor will want to see you about 3 to 6 weeks after an IUD has been inserted to check whether you are experiencing any side effects. They may want to check the position of the IUD by checking the string. In some cases, a pelvic ultrasound scan may be recommended to check the position of the IUD.
You should see your doctor for a yearly check-up while using an IUD.